Unified Provider Data Ingestion
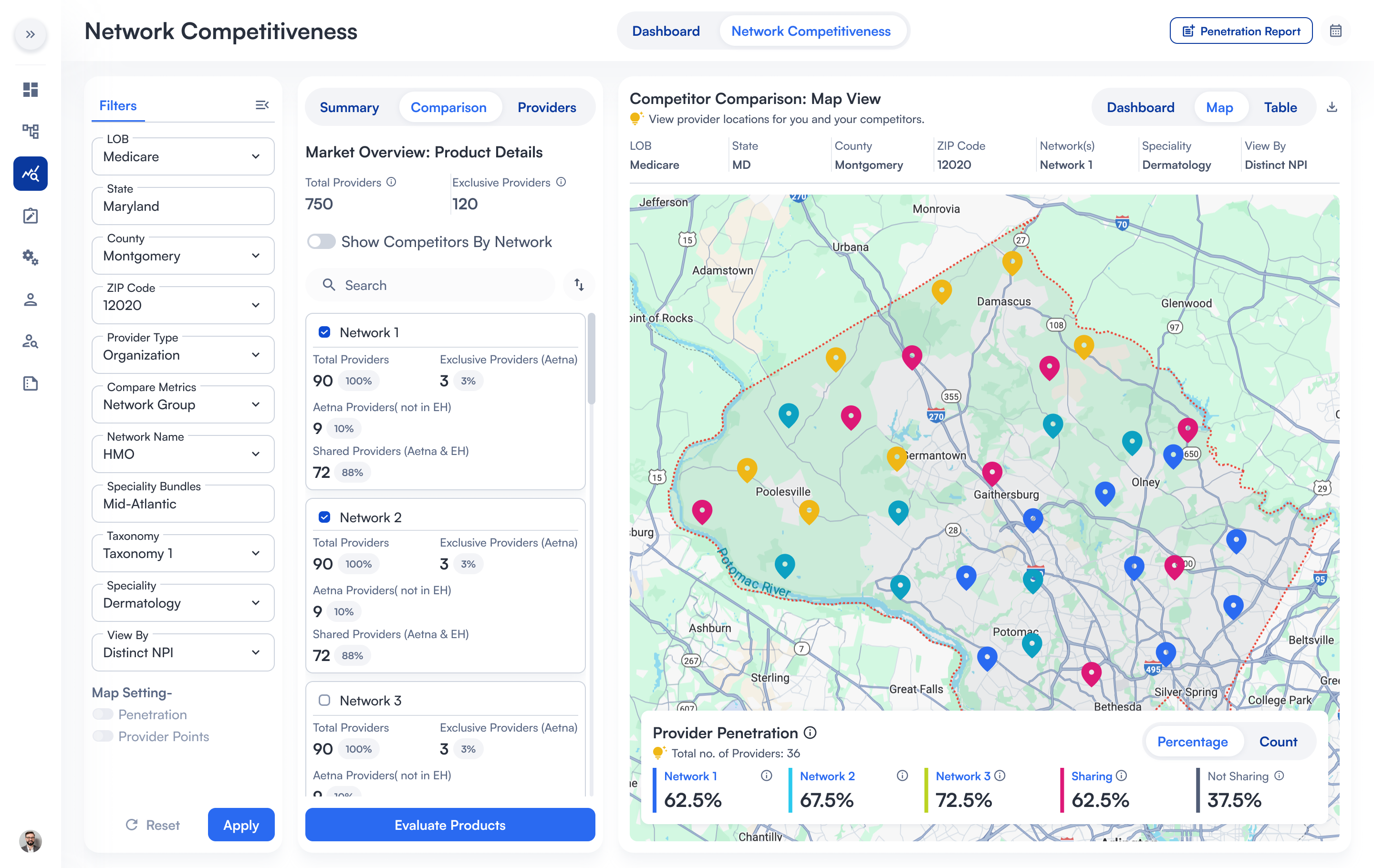
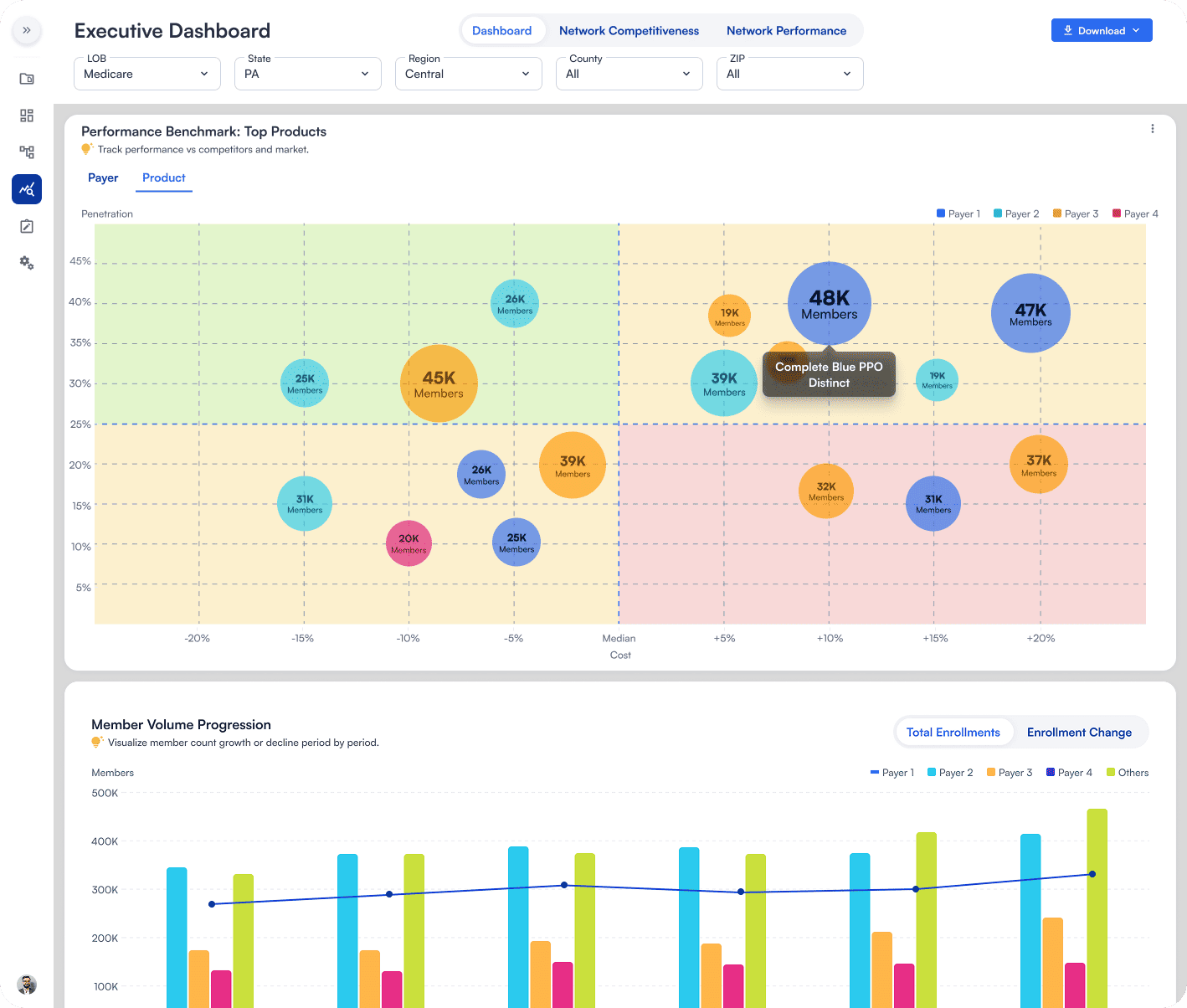
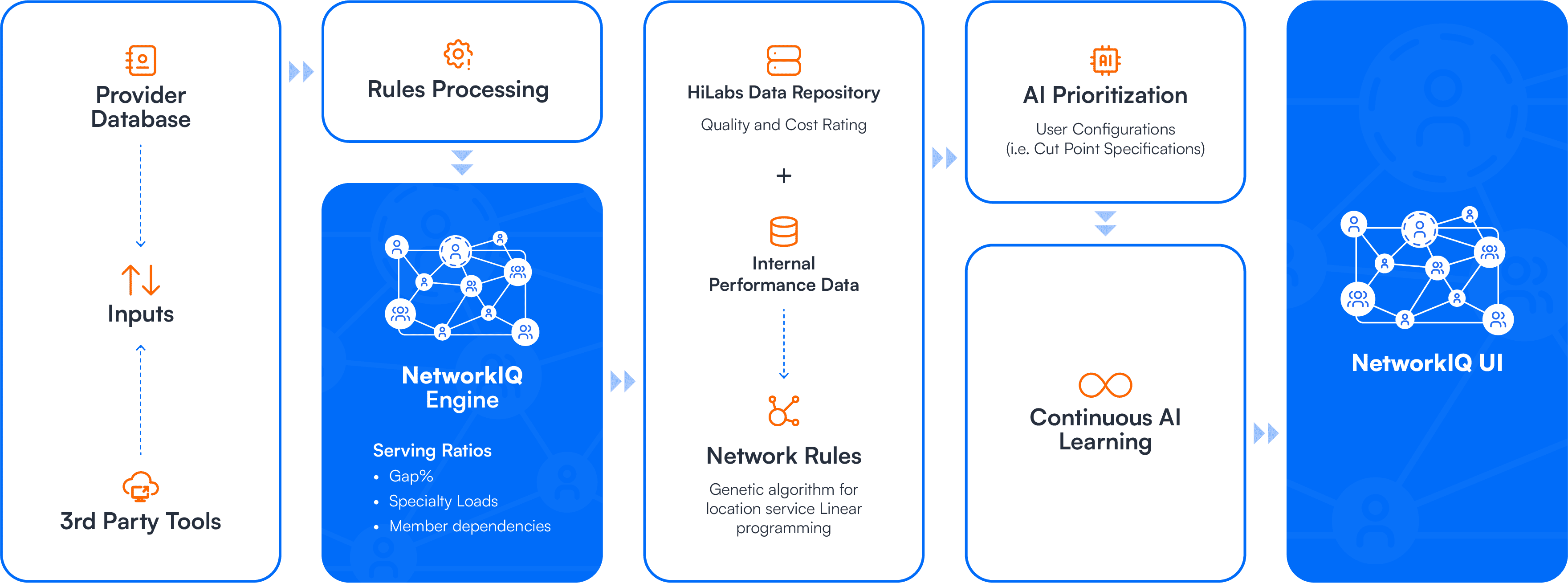
NetworkIQ integrates data from internal systems, credentialing feeds, claims and utilization files, and other third-party sources. A unified data pipeline reconciles these inputs, so health plans can rely on a single, consistent provider dataset.